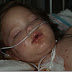
Lucy’s fevers have come down, she continues to hover around 100.8 to 101.2 degrees. Motrin is working beautifully to bring the fevers down, but now it is her belly that is acting “off”. She is not interested in eating any Cheerios, she even put one in her mouth only to take it right back out…so uncharacteristic for our little Cheerio addict. When speaking yesterday with Dr. R, the diagnostic referral doctor, he was not at all surprised that she was having slower motility. Her body is busy fighting off whatever bugs have invaded her, and the limited energy that she has is being reallocated for her current needs. We have switched her feeds from being 22 hour continuous, to being a few hours on and a few hours off. I have cut back her feeding rate in hopes of keeping her nourished and hydrated, but also more comfortable. Since we made this change to her “normal” feeding schedule we are checking her glucose regularly to ensure that we don’t have it fall too low. Continuous feeders, like Lucy, don’t experience the ups and downs in their insulin levels because they are constantly receiving nutrients. Their bodies don’t know how to dip into their glycogen storage because of this, thus they are more prone to having their glucose drop too low which could put her into crisis. As long as Lucy continues to receive enough nutrients, her glucose stays within normal limits, and she continues to wet her diapers we feel comfortable with this feeding schedule. I did turn her pump back on this morning at 3:00am and she has been running ever since at a slower rate, but continuously…so maybe, just maybe, things are improving (I wrote this at 8:30am, but am just getting around to posting it at 9:30pm).
Our appointment with Dr R was what we hoped it would be. He is a specialists who takes on complex cases such as ours. He is willing to be Lucy’s doctor for whatever needs she has. He can coordinate her care between specialists in the DuPont system and try to coordinate her care with her CHOP doctors as well, I say good luck with that one. If and when she gets admitted to the hospital he could be her main doctor, thus eliminating all of the interns, residents, and fellows. At this point we are trying to cut out some of the doctors in her life, no offence to any of Dr. F’s med students who read this, but the fewer docs the easier for us. He is very knowledgeable about mitochondrial disease he even attended the UMDF’s conference last year, but is not a “mito specialist.” He does have a very good relationship with Dr. Shoffner and consults with him on many of his mito patients. In fact, he is going to contact him this week in regards to some of the tests that are still pending from Lucy’s muscle biopsy, in particular her genetics testing. If, and this is a BIG if, they are able to find the genetic mutation that is causing Lucy’s disease than we may be able to test our other kids blood to see if they have or carry the same gene mutation.
I have not written much about this, but we have our suspicions that Sophie is affected with a milder form of the same disease. Sophie was diagnosed with failure to thrive when she was six months old, but at around eighteen months she recovered, well I might add. She was always on the late end of the developmental spectrum, but never “delayed”. She didn’t start talking until she was closer to two and has not stopped since! Sophie struggles with chronic constipation and bloating, this is affecting her/our daily lives but we manage. Dr Shoffner felt that in addition to all of Lucy’s issues, having two babies diagnosed FTT was even more compelling evidence to test for mitochondrial disorders. To be honest, I am afraid to find out our genetics, but knowing would be beneficial. It would allow us to test Sophie without having to do a muscle biopsy. Because of the complexities of this disease there are varying degrees of severity, no two patients present the same even when they have the same genetic mutation.
Our world has not been the same since Lucy was born…actually since any of our kids were born.







Post Comment
I hope Lucy feels better soon. These fevers are so tough on our kids!
I don't know if I have mentioned this to you or not, but we think that Emma has a mild form of this disease as well. Several therapists have noted her low tone, and a geneticist has gone as far as to say that she definitely has a mild form of mito merely based on her low tone, short stature, facial features (go figure!) and energy issues. In my heart, I know that she does, but we do not at all plan to test her unless she shows more defined symptoms.
This disease is tough sometimes. Love your posts...
I know the pain you and Amber express when we talk about sibling and this disease. Its not something I discuss on Jacks blog because it involves our 15 yr old daughter. She also has a history of dev delays, FTT, feeding difficulties, and still the hypotonia, exercise intolerance, fatigue, reflux, low blood pressures (black-outs)
I just dont want her to read anything scary right now. As it is, she worries about her brother and how long he will be with us. I mean she's old enough to google and see how devastating Mito is anyway...but dont need to further her fears by talking about her medical issues and the probability of her also having this disease as well. I know someday we'll have to have a more serious conversation with her but she's just started Highschool and busy being a teen right now with all that comes with that. For now, we're praying she continues to remain stable.
I also fear the testing and finding out someday how Mito may affect our family. Its just too much for me to think about though. I know Im symptomatic now too but I worry more about our kids naturally. Yep, this disease is tough. I wish just one day I wouldnt have to think about it, sigh.
BIG hugs to your dear girl, I hope these fevers resolve soon, poor kiddo. thinking about your guys tonight-
Heidi & Jack.
Glad you got to hang out with out main man! Love that guy -- he will take good care of you guys!
I was just directed to your blog. I have two children who died, from suspected mito disease. We have living children, primarily my two youngest, who have symptoms of mito. I am wondering what genetic test you're referring to. We had a blood test last year, I think mtDNA 3000 that didn't give us any answers. But we just did a new draw for the whole mtDNA genome panel. I'm not sure if I'm getting these names right, but we are waiting for results. Our two children who died had crisis events in infancy. Our youngest is now 21 months old, so we are glad to have our living children be older. But more and more there are symptoms that have me constantly wondering if mito disease is going to take the life of another child of mine. I guess I'm impatiently looking for support because I am afraid of the results telling us what we are really facing, and I'm also afraid that the test will be inconclusive like all the other tests. Both of our kids who died had muscle biopsies and extensive testing, including genetics testing, and complete autopsies, but we don't have a real direction to go other than highly suspected mito disease. I'm rambling. I hope you don't mind me posting on your blog. I just really would like a diagnosis. I posted on my blog about a year after my daughter Bridget died, about the power in having a diagnosis: http://jobs-apprentice.blogspot.com/2008/09/and-out-of-ground-lord-god-formed-every.html Maybe it's the greener on the other side. Has a diagnosis helped you? Better stop rambling. I have too many questions and anxiety, so I just ramble. Thank you for your blog posts and sharing about your family so that others who are trying to make sense of medical complexities in their own families have a place to learn and feel less alone.
Post a Comment